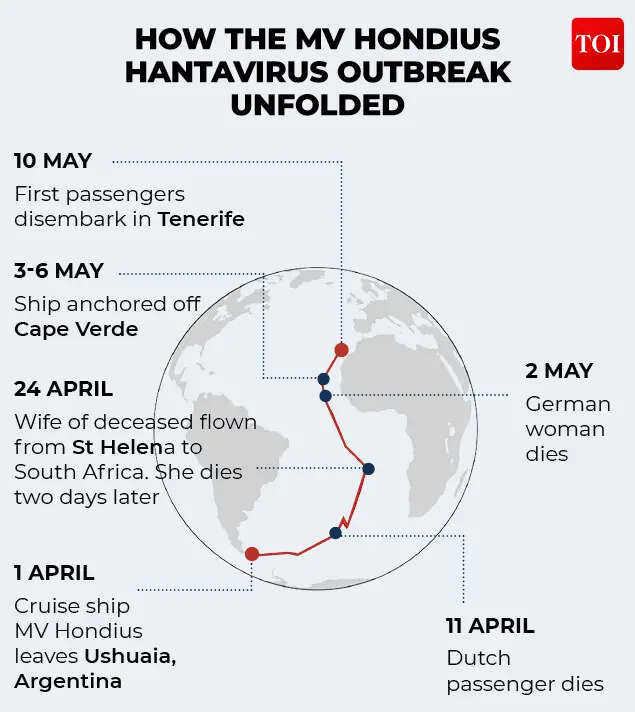
Departing from Ushuaia, Argentina, on April 1, the MV Hondius set sail on the “Atlantic Odyssey”, a 33-day voyage envisioned as the pinnacle of expedition cruising for nature enthusiasts. Destined for Praia, Cape Verde, the vessel was charted to traverse the world’s most desolate reaches, including South Georgia, Tristan da Cunha, and St Helena.However, this ambitious trek across the South Atlantic soon descended into a harrowing case study in 21st-century epidemiology.The nightmare started unfolding on April 6, when a 70-year-old Dutch passenger first reported feeling unwell. His initial symptoms were deceptively common. A high fever, severe headache, and mild diarrhea. For five days, his condition fluctuated until April 11, when he suffered a sudden and catastrophic onset of respiratory distress. He died in his cabin that evening while the ship was still at sea. At the time, the cause of death remained a mystery, but the situation rapidly escalated when the ship reached the remote island of St. Helena on April 24. The atmosphere on board shifted instantly from wonder to dread.Turkish YouTuber Ruhi Çenet, who disembarked that day, later described the chilling uncertainty to The New York Times. “Everyone was shocked,” Çenet recalled, noting that while the crew tried to maintain calm, the gravity of the situation was visible. “Initially, I thought there was just a fever going around, but after observing the lady, the Dutch man’s wife, struggling with her condition, I thought it was better to stay in my room than take any risk.”His instincts proved tragically correct. On April 24, the woman disembarked at St. Helena with her husband’s body and boarded a flight to South Africa, where she collapsed in Johannesburg and died two days later. By sequencing and matching the viral strains from the victims, South African virologists provided definitive evidence of human-to-human transmission during the voyage. A third victim, a German woman who remained on the ship, succumbed to acute pneumonia on May 2, marking the third fatality and confirming that the vessel was still an active site of infection.
.
As the death toll climbed, the luxury cruise ship was transformed into a floating isolation vessel, a modern-day “ghost ship” carrying passengers infected with the deadly hantavirus, a situation that may have left many nations wary of allowing it to dock, until Spain finally extended a gesture of humanity for the safety and dignity of those who had remained stranded on board for days, even as regional authorities hesitated. As of mid-May 2026, the outbreak of the Andes strain of hantavirus had claimed at least three lives and triggered a multi-continent health investigation. The tragedy traced back to the Dutch couple, avid birdwatchers who had spent the weeks leading up to April 1 traversing the rugged landscapes of Argentina, Chile, and Uruguay. Investigators believe they were likely exposed to the virus at a site near a landfill in South America where rodent populations thrive, unknowingly carrying the pathogen aboard the vessel when it departed from Ushuaia.What has placed the World Health Organization on high alert is the identification of the Andes virus, a particularly dangerous variant of hantavirus. Unlike most strains that are strictly zoonotic, the Andes strain is one of the few capable of limited human-to-human transmission through prolonged, close contact. Confirmed or “probable” cases have since been identified in passengers and crew from the UK, Switzerland, France, Spain, and the Netherlands, including the ship’s own doctor, who had to be medically evacuated. The outbreak aboard the Hondius also reflects a wider environmental trend unfolding in Argentina, where hantavirus cases have nearly doubled this season, reaching 101 confirmed infections and 32 deaths. Scientists increasingly link these shifts to climate change, which is altering rainfall cycles, temperatures, vegetation growth, and rodent behaviour across vulnerable regions. Warmer winters and erratic rainfall patterns have triggered massive “masting” events, sudden explosions in seed production that dramatically increase food availability for rodents, allowing populations of the long-tailed pygmy rice rat, a known carrier of the Andes virus, to rapidly expand. Experts warn that as climate-driven ecological disruption intensifies and human activity continues to encroach on natural habitats, the barrier between people and infected rodents is steadily eroding.In order to understand why scientists are increasingly linking hantavirus outbreaks to climate change, it is important to first understand what the virus is, how it spreads, and why changing ecosystems are creating new opportunities for human exposure.
What is Hantavirus? A rodent-borne virus named after a Korean river
According to the WHO, hantaviruses are a group of zoonotic viruses carried primarily by rodents that can cause severe and sometimes fatal disease in humans. People are typically infected through contact with infected rodents or by inhaling particles contaminated with their urine, droppings, or saliva. Once transmitted to humans, hantaviruses can lead to a spectrum of illness, ranging from relatively mild disease to severe, life-threatening conditions.
.
In the Americas, infection is most commonly associated with hantavirus cardiopulmonary syndrome (HCPS), a rapidly progressing respiratory illness that can affect the lungs and heart and carries a case fatality rate of up to 50%. In Europe and Asia, hantaviruses more commonly cause haemorrhagic fever with renal syndrome (HFRS), which primarily affects the kidneys and the vascular system. The Andes virus, found in South America, in which rare instances of possible human-to-human transmission have been documented, primarily in close-contact or caregiving settings There is currently no specific antiviral treatment or cure for hantavirus disease. Clinical management is therefore entirely supportive, focusing on early hospitalisation, intensive monitoring, and management of respiratory, cardiac, and renal complications, interventions that can significantly improve survival when provided in time. The name “hantavirus” originates from the Hantan River in South Korea, where Korean virologist Lee Ho-wang and his team first isolated the virus in 1978 from the striped field mouse (Apodemus agrarius), naming it Hantaan virus after the region. However, the disease was recognised long before its discovery. During the Korean War (1951–1954), more than 3,000 United Nations soldiers were affected by a mysterious illness known as Korean hemorrhagic fever, later identified as HFRS.
How climate change fuels Hantavirus risk
Hantavirus outbreaks are closely linked to environmental conditions that influence rodent population dynamics. One of the clearest examples is the 1993 Four Corners outbreak in the United States, which followed an intense El Niño event in 1992–1993. Increased rainfall during this period led to a surge in vegetation growth, including pinyon pine nut production, a key food source for deer mice. This sudden abundance of food triggered a rapid increase in rodent populations, which in turn raised the likelihood of human exposure to infected animals and contaminated environments. Similar patterns have been observed in other regions and time periods, where fluctuations in rainfall, temperature, and ecosystem productivity influence rodent abundance and disease risk. Because hantaviruses are maintained in specific rodent hosts, changes in host population density directly affect the potential for spillover into human populations.
.
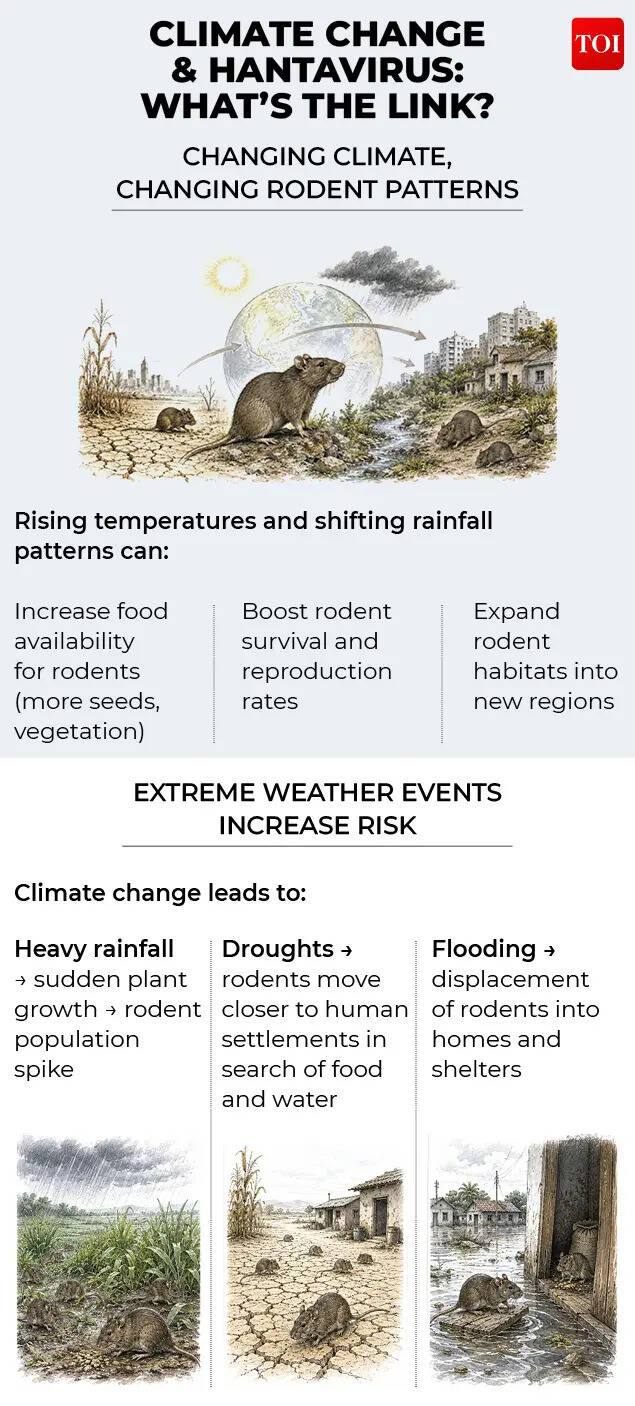
“Change in climate may impact rodent borne disease risks over time by changing pattern of rainfall, temperature, availability of foods, and rodent movements as well. Heavy rains, floods, warmer conditions and urban expansions can also push rodents closer to homes and storage spaces ultimately increasing human exposure,” Dr. Arvind Kumar Aggarwal of Sri Balaji Action Medical Institute told TOI.“In India, this does not mean a confirmed hantavirus surge, but it does suggest the need for stronger surveillance of rodent-borne infections. Other factors such as better sanitation, rodent monitoring, and climate sensitive disease tracking will become increasingly significant for public health preparedness,” he added.Researchers caution that climate change does not directly cause hantavirus outbreaks, but it can increase the frequency or geographic spread of ecological conditions that support rodent population booms and greater human exposure. Overall, evidence suggests hantavirus risk is strongly shaped by environmental conditions, with climate acting as an indirect but important driver through its influence on rodent ecology and human contact patterns.
Indigenous knowledge and scientific investigation in the Four Corners outbreak
According to the American Society of Microbiology, Indigenous knowledge played a significant role in helping investigators understand the unusual respiratory outbreak in the Four Corners region of the United States in the early 1990s. Diné elders and healers observed that similar clusters of severe illness had appeared in earlier years, often following periods of unusually high rainfall. These observations were consistent with historical patterns linked to environmental change, where increased precipitation led to greater availability of food sources such as pinyon pine nuts, supporting rapid growth in rodent populations, particularly deer mice.In Navajo tradition, humans and rodents are understood to belong to different natural domains, and imbalance between these worlds is seen as a potential source of illness. Elders had long advised caution around deer mice and prairie dogs and recommended avoiding contact with their waste, including contaminated dust and materials in enclosed spaces. When CDC investigators arrived in the region, discussions with tribal elders provided important contextual insight into the timing and ecological conditions surrounding the outbreak. This information helped researchers connect the sudden increase in rodent populations with the emergence of unexplained respiratory deaths. Combined with clinical observations and international experience with similar syndromes in Europe and Asia, this collaboration contributed to the hypothesis that a previously unidentified hantavirus was responsible.
Hantavirus in India: first serological evidence
According to the 2008 study “Seroepidemiological study on hantavirus infections in India” by Sara Chandy et al., published in the Transactions of the Royal Society of Tropical Medicine and Hygiene, researchers found early serological evidence suggesting that hantaviruses were circulating in India despite no previously documented clinical cases.The multi-institutional study evaluated 661 individuals from potential high-risk groups in Tamil Nadu, including patients with chronic renal disease, warehouse workers, and members of the Irula tribal community engaged in traditional rodent trapping. Using ELISA, immunofluorescence assays, and Western blot confirmation, researchers identified 38 seropositive samples, of which 28 were confirmed positive for anti-hantavirus IgG antibodies.

.
The Irulas, historically known for catching snakes and rats, were considered particularly vulnerable because of frequent exposure to rodent reservoirs. Researchers noted that hantaviruses are carried by rodents without causing illness in the animals themselves, while humans become infected mainly through inhalation of aerosolised particles contaminated with rodent urine, saliva, or droppings , especially in poorly ventilated or rodent-infested environments.The findings suggested the possible circulation of hantavirus strains related to Seoul, Thailand, and Hantaan viruses in India. Researchers cautioned that limited diagnostic awareness may have led to under-recognition of infections and called for stronger surveillance and molecular studies to better understand circulating strains and their rodent hosts.Importantly, the study stressed that seropositive results only indicate previous exposure to hantaviruses or related strains at some point in time. The presence of antibodies alone does not necessarily mean an active infection, severe illness, or the ability to transmit the virus.
What do doctors say?
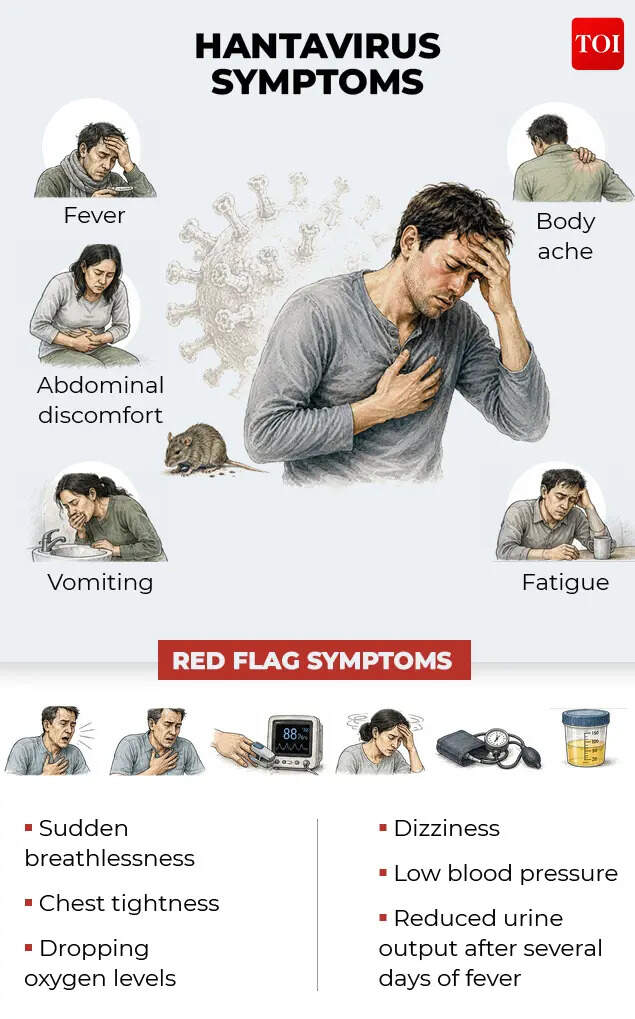
Doctors also caution that early symptoms can initially resemble common viral illnesses, making awareness important in high-risk exposure settings. Fever, body ache, fatigue, vomiting, and abdominal discomfort may precede more dangerous signs such as sudden breathlessness, chest tightness, dropping oxygen levels, low blood pressure, or reduced urine output.“In severe cases, hantavirus can lead to Hantavirus Cardiopulmonary Syndrome, a rapidly progressive and potentially fatal condition affecting the lungs and circulation,” said Dr. Arvind Kumar Aggarwal of Sri Balaji Action Medical Institute. He emphasized that early diagnosis and supportive critical care remain the most important factors influencing survival.Because no approved vaccine or specific antiviral treatment currently exists for routine use, treatment focuses on supportive care, including oxygen therapy, intravenous fluids, blood pressure support, monitoring of kidney and lung function, and intensive care management when necessary.

.
Despite growing global concern over the Andes strain outbreak linked to the Hondius voyage, Indian doctors stress that hantavirus does not currently pose the kind of widespread public-health threat associated with respiratory pandemics such as COVID-19.“There is no evidence of any large community-level outbreak in India at present,” said Dr. Radhika Arvind Ghongane, Consultant Pulmonologist at SPARSH Hospital in Bengaluru. However, she noted that earlier Indian studies had suggested prior hantavirus exposure among individuals living or working in close proximity to rodents.According to Dr. Ghongane, the risk remains relatively higher in rodent-prone settings such as farms, grain storage facilities, warehouses, construction sites, and poorly ventilated spaces with poor sanitation. “There is no reason for public panic,” she said. “Hantavirus remains an uncommon infection in India, but awareness and preventive hygiene are important.”“One important precaution is to avoid dry sweeping or vacuum cleaning rodent droppings, as this can release infectious particles into the air,” Dr. Ghongane explained. She added that one of the biggest misconceptions is the belief that hantavirus spreads easily from person to person. “In reality, most hantavirus strains do not transmit through casual human contact. The infection is mainly linked to environmental exposure to rodents rather than community transmission.”Public-health precautions therefore focus largely on rodent control and safer cleaning practices. Experts recommend ventilating closed rooms before cleaning, wearing gloves and masks, disinfecting contaminated surfaces with bleach solution, and avoiding activities that stir contaminated dust into the air.Includes inputs from reports by The Guardian, AP, and CNN






